This blog is in response to the COVID-19 pandemic. Risk management in any business is of utmost importance and ensuring the safety of our patients and staff is our top priority. This is our response which will play a role in alleviating pressure on our hospitals in the form of social distancing and assisting with dental emergencies in our local community. This will be achieved by defining essential and non-essential dental treatment, triaging, screening, hygiene and infection control audits and waste management.
“Up to now, there has been no consensus on the provision of dental services during the epidemic of COVID-19. On the basis of our experience and relevant guidelines and research, dentists should take strict personal protection measures and avoid or minimize operations that can produce droplets or aerosols.”
https://journals.sagepub.com/doi/full/10.1177/0022034520914246
Operations that produce the most amount of droplets and aerosols are scale and cleans which our team has classified as non-essential treatment. This is followed by restorative work using the triplex syringe and high/slow speed drill handpieces.
“The participants in dental practice expose to tremendous risk of 2019-nCoV infection due to the face-to-face communication and the exposure to saliva, blood, and other body fluids, and the handling of sharp instruments. Dental professionals play great roles in preventing the transmission of 2019-nCoV.”
https://www.nature.com/articles/s41368-020-0075-9
Social Distancing
Riverstone Family Dental will assist in slowing the spread of COVID-19 by implementing social distancing in the following ways:
- Defining essential and non-essential treatment.
- Essential and emergency treatment only until further notice.
- Existing patients will be prioritised to minimise travel and to assist with social distancing for our local community.
- Walk-ins will not be accepted. Please call the clinic to make a booking or an enquiry.
- During treatment hours, the clinic door will be closed with a sign “Patient Treatment in Progress”.
- One person at a time – only the patient who is booked in may present to the clinic with a maximum of one guardian/parent if it is a child.
Dental Emergencies
Riverstone Family Dental will be on standby for dental emergencies in our local community until further notice. Our already strict infection control protocols have now been increased. To allow for this, a limited number of patients can be seen per day to allow time for appropriate decontamination.
“it was shown at room temperature that 2019-nCoV remains infectious from 2h up to 9 days, and persists better at 50% compared with 30% relative humidity. Thus, keeping a clean and dry environment in the dental office would help decrease the persistence of 2019-nCoV.”
https://www.nature.com/articles/s41368-020-0075-9
Our updated decontamination protocols for environmental cleaning and disinfection procedures will include regular use of strong disinfectants and detergents on equipment, furnishings, floors, handles, cupboards and instruments before and after every patient. You may have noticed the removal of the toy section in our reception area which was done in early February 2020. Please advise staff if you suffer from allergies or intolerances to certain products.
Our team will favour the use of extraoral xrays such as panoramic (OPG) radiographs over intraoral ones in order to minimise saliva production and potential to cause cough/gag reflex. Patients will be screened as to whether they have a cough or gag reflex so our team can minimise the release of droplets during the dental appointment.
“extraoral dental radiographies, such as panoramic radiography and cone beam CT, are appropriate alternatives during the outbreak of COVID-19.”
https://journals.sagepub.com/doi/full/10.1177/002203452091424
Essential vs Non-Essential
Riverstone Family Dental has a list of essential and non-essential treatment in place. Our team will designate a specific number of appointments per day and allocate those appointments based on how urgent or essential that treatment is for that particular patient. Patients will be placed on a standby list and will be contacted and triaged over the phone prior to scheduling their appointment.
|
Essential |
Non-essential |
| Moderate/severe decay needing a filling | Mild decay needing a filling |
| Fractured tooth causing pain | Fractured tooth not causing pain |
| Active infection/swelling/pain | Crowns/bridges/veneers |
| Extractions of teeth causing pain | Scale and cleans, recall appointments |
| Ongoing Invisalign monitoring | Asymptomatic wisdom teeth |
| Root canal treatment where patient is in pain or to finalise course of treatment | Implants |
| Periodontal treatment in patients with diabetes or cardiac diseases | Starting denture treatment |
| Ongoing denture treatment |
Triaging
“Patients with fever should be registered and referred to designated hospitals. If a patient has been to epidemic regions within the past 14 d, quarantine for at least 14 d is suggested. In areas where COVID-19 spreads, nonemergency dental practices should be postponed.”
Kohn et al. 2003; Li et al. 2004; Samaranayake and Peiris 2004
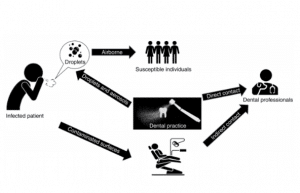
“The pathogenic microorganisms can be transmitted in dental settings through inhalation of airborne microorganisms that can remain suspended in the air for long periods, direct contact with blood, oral fluids, or other patient materials, contact of conjunctival, nasal, or oral mucosa with droplets and aerosols containing microorganisms generated from an infected individual and propelled a short distance by coughing and talking without a mask , and indirect contact with contaminated instruments and/or environmental surfaces. Infections could be present through any of these conditions involved in an infected individual in dental clinics and hospitals, especially during the outbreak of 2019-nCoV.”
Kampf et al. 2020; Chen et al. 2020; Cleveland et al. 2016; Harrel et al. 2004; Liu et al. 2011
https://www.nature.com/articles/s41368-020-0075-9
Triaging patients will allow us to screen people who may be likely to have COVID-19. This is achieved by studying research papers which outline the proposed source and transmission of COVID-19. This is what we know so far:
This virus is transmitted through people who may or may not be showing symptoms. Incubation time can be 4-14 days which means, a person is infected but may not yet be showing symptoms. Literature suggests that during the incubation period, there is a chance this person can infect others. The mode of transmission of this virus is mainly via respiratory droplets (cough, sneeze) and contact transmission. Definitions about airborne transmission are inconsistent.
“In addition to the infected patient’s cough and breathing, dental devices such as high-speed dental handpiece uses high-speed gas to drive the turbine to rotate at high speed and work with running water. When dental devices work in the patient’s oral cavity, a large amount of aerosol and droplets mixed with the patient’s saliva or even blood will be generated. Particles of droplets and aerosols are small enough to stay airborne for an extended period before they settle on environmental surfaces or enter the respiratory tract. Thus, the 2019-nCoV has the potential to spread through droplets and aerosols from infected individuals in dental clinics and hospitals.”
https://www.nature.com/articles/s41368-020-0075-9
*** Patients should expect phone triaging and further screening upon presentation to the clinic. Riverstone Family Dental staff have a list of questions and protocols to follow.
Hygiene and Infection Control
Hand hygiene – hand sanitiser will be placed at the reception counter. Patients will be asked to use this upon entering and leaving the clinic.
Our staff are already trained in hand hygiene and hold Hand Hygiene certificates. The following recommendations will be reinforced:
“Specifically, the oral professionals should wash their hands before patient examination, before dental procedures, after touching the patient, after touching the surroundings and equipment without disinfection, and after touching the oral mucosa, damaged skin or wound, blood, body fluid, secretion, and excreta. More caution should be taken for the dental professionals to avoid touching their own eyes, mouth, and nose.”
https://www.nature.com/articles/s41368-020-0075-9
A pre-op mouth rinse consisting of chlorhexidine and either 1% hydrogen peroxide or 0.2% povidone will assist in killing a broad range of microbes, including viruses.
During treatment, our team will be protected with PPE (Personal Protective Equipment) and use rubber dams where possible and high-volume saliva ejectors in order to minimize aerosol or spatter in dental procedures. Our team will also try as much as possible to minimise droplets or aerosols – where this is impossible, we will strategically schedule these procedures at the end of the day.
Handling waste
“The medical and domestic waste generated by the treatment of patients with suspected or confirmed 2019-nCoV infection are regarded as infectious medical waste. Double-layer yellow color medical waste package bags and “gooseneck” ligation should be used. The surface of the package bags should be marked and disposed according to the requirement for the management of medical waste.”
https://www.nature.com/articles/s41368-020-0075-9
Where suspected COVID-19 cases are treated, their treatment waste will be disposed of in the clinic’s contaminated waste bin. All equipment will be autoclaved using the clinic Class B steriliser as per Riverstone Family Dental Infection Control Protocols.
***Please note this is a new viral pandemic and this information is valid at the time and date of writing on 18th March 2020. This is a rapidly developing situation and we are monitoring closely and will try to keep you updated.***
Further Information
Coronavirus COVID-19 Global Cases by the Center for Systems Science and Engineering (CSSE) at Johns Hopkins University (JHU)
https://gisanddata.maps.arcgis.com/apps/opsdashboard/index.html#/bda7594740fd40299423467b48e9ecf6
NSW Health
https://www.health.nsw.gov.au/Infectious/diseases/Pages/coronavirus.aspx
Coronavirus Disease 2019 (COVID-19): Emerging and Future Challenges for Dental and Oral Medicine
https://journals.sagepub.com/doi/full/10.1177/0022034520914246
Transmission routes of 2019-nCoV and controls in dental practice
www.nature.com/articles/s41368-020-0075-9
EARLY THOUGHTS ON A PANDEMIC – A Conversation with Amesh Adalja. Amesh Adalja, MD, is an infectious disease specialist at the Johns Hopkins University Center for Health Security. His work is focused on emerging infectious disease, pandemic preparedness, and biosecurity.
https://samharris.org/podcasts/191-early-thoughts-pandemic/
HOW SHOULD WE RESPOND TO CORONAVIRUS? A Conversation with Nicholas Christakis. Nicholas A. Christakis, MD, PhD, MPH, is the Sterling Professor of Social and Natural Science at Yale University, where he directs the Human Nature Lab and is the Co-Director of the Yale Institute for Network Science.
https://samharris.org/podcasts/190-respond-coronavirus/
Coronavirus: Why You Must Act Now. Politicians, Community Leaders and Business Leaders: What Should You Do and When? Tomas Pueyo MSc in Engineering. Stanford MBA. Ex-Consultant.
https://medium.com/@tomaspueyo/coronavirus-act-today-or-people-will-die-f4d3d9cd99ca
Coronavirus – When Should You Close Your Office?
https://docs.google.com/spreadsheets/d/17YyCmjb2Z2QwMiRRwAb7W0vQoEAiL9Co0ARsl03dSlw/edit#gid=0
Response to COVID-19 in Taiwan. Big Data Analytics, New Technology, and Proactive Testing
https://jamanetwork.com/journals/jama/fullarticle/2762689
Why outbreaks like coronavirus spread exponentially, and how to “flatten the curve”
https://www.washingtonpost.com/graphics/2020/world/corona-simulator/
Kohn, WG, Collins, AS, Cleveland, JL, Harte, JA, Eklund, KJ, Malvitz, DM; Centers for Disease Control and Prevention. 2003. Guidelines for infection control in dental health-care settings. (2003). https://www.cdc.gov/mmwr/preview/mmwrhtml/rr5217a1.htm
Li, R, Leung, K, Sun, F, Samaranayake, L. Severe acute respiratory syndrome (SARS) and the GDP. Part II: implications for GDPs. Br Dent J. 197(3):130–134. (2004).
Samaranayake, LP, Peiris, M. Severe acute respiratory syndrome and dentistry: a retrospective view. J Am Dent Assoc. 135(9):1292–1302. (2004).
Kampf, G., Todt, D., Pfaender, S. & Steinmann, E. Persistence of coronaviruses on inanimate surfaces and its inactivation with biocidal agents. J. Hosp. Infect. (2020). https://doi.org/10.1016/j.jhin.2020.01.022
Chen, J. Pathogenicity and transmissibility of 2019-nCoV—a quick overview and comparison with other emerging viruses. Microb. Infect. (2020). https://doi.org/10.1016/j.micinf.2020.01.004
Cleveland, J. L. et al. Transmission of blood-borne pathogens in US dental health care settings: 2016 update. J. Am. Dent. Assoc. (1939) 147, 729–738. (2016).
Harrel, S. K. & Molinari, J. Aerosols and splatter in dentistry: a brief review of the literature and infection control implications. J. Am. Dent. Assoc. (1939) 135, 429–437. (2004).
Liu, L. et al. Epithelial cells lining salivary gland ducts are early target cells of severe acute respiratory syndrome coronavirus infection in the upper respiratory tracts of rhesus macaques. J. Virol. 85, 4025–4030. (2011).